Feel in charge of your skin
PERSONALISED DERMATOLOGY TREATMENT PLANS
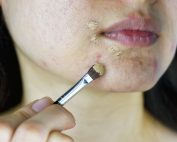
Genital dermatoses (or skin conditions that affect the genital area) can cause much discomfort and sometimes embarrassment
THESE CONDITIONS INCLUDE LICHEN SCLEROSUS, LICHEN PLANUS, ECZEMA AND PSORIASIS. IN THIS PAGE, I EXPLAIN THE SYMPTOMS AND CAUSES OF GENITAL DERMATOSES – AND HOW I TREAT THEM
Treatment helps people of all ages take control of their skin condition and get their life back.
How do genital dermatoses impact people on a day-by-day basis?
THE DISCOMFORT CAN NOT ONLY BE PHYSICAL, BUT CAN ALSO IMPACT YOUR PERCEPTION OF YOURSELF AND YOUR SOCIAL LIFE
Symptoms of skin problems affecting the genitals include…
In some conditions, such as lichen sclerosus and lichen planus, the skin can progressively scar and lead to the fusion of the labia in women and phimosis (difficulty in retracting the foreskin) in men. Lichen planus can result in ulceration in the affected areas in both the vulval and vaginal region in women and the glans penis in men.
How does it feel?
You might experience itching, pain and inflammation of the affected skin and mucosal surfaces. You might feel pain when urinating and opening your bowels. You might experience pain during and following sexual intercourse, often resulting in trauma and small cracks to the affected skin.
Certain individuals may experience psychosexual difficulties
These can be due to either anticipation of pain and discomfort during sexual intercourse, or due to concerns regarding the appearance of the affected skin.
It can affect your mood and social life
Some people may experience an impact on their mood and social life due to the perception of stigma because the condition affects the genital skin.
Is there a cure?
Unfortunately, these types of skin problems are chronic. That means that they can flare up from time to time. Therefore, we need to treat them appropriately. Careful management of the condition should allow you to be symptom-free and reduce the number of flare ups you get in future to a minimum.
What my patients love about my service
MY PATIENTS ARE MY BEST PROMOTERS

Please pass on my thanks to Dr Pratsou for her assessment on my continued taking of roaccutane.She was completely right, I didn’t need a new course, I needed to move away from the drug. The creams she gave me and Cetaphil recommendation have meant my skin has been the best it’s ever been (ongoing and since I saw her) ALL SUMMER :))))) I’ve had zero problems…and I’m loving it.
Thank you once again.

“Dear Dr Pratsou,
Following the consultation today I feel it appropriate to say thank you for your help in dealing with my rosacea.
On each occasion, I have visited your department I have noticed the kindness and cheeriness of all the staff I have encountered and particularly wanted to say that you made me feel at ease with your calmness and excellent manner.
All is much appreciated.”

“Thank you very much!!
You three were (and are) a great team!
I will remember you.
You made me feel comfortable.”

“Tania,
Please pass to Dr Pratsou my thanks for her skilled work.
The wound is healing beautifully and now the stitches are out it looks as though it will be almost invisible once fully healed.”

“Dear Dr Penelope, Rena & the team, (I can’t remember the nurse’s name who helped me during my 2 procedures at the Spire!)
I wanted to thank you for your support and help during a very difficult time. You guys do a wonderful job – and we are eternally grateful for your help.”

“I would like to put on record how impressed I was with the operation you performed for the removal of the SCC on my neck. I cannot even see where the cut or the stitches were! I am indeed very grateful for the excellent work you do.”

“Dear Dr Pratsou,
I am very grateful to you for your diagnosis, recommended treatment and advice. Your letter to my GP sets out both the course of events, and your own analysis of probable condition and possible cause, clearly summarising our discussion.
I hope there will be no recurrence but I will certainly come back to you if there is.”

“Dear Tania,
Please pass on my thanks to Dr Pratsou. I saw her this morning for a mole check. She was so lovely and reassuring. Please also thank the two nurses who assisted her during the mole removal procedure. I was very nervous, but they were very efficient, which meant I did not have too long to think about it, but most of all they were very kind. They kept me distracted and calm, which made a huge difference. Thank you also for your efficiency in both booking me in so quickly.”

Dear Ms. Pratsou,I am writing to thank you for the care you have given me in the past few months. From the moment I walked into your consulting room with a lesion on my cheek, a lesion that I fully expected to be some sort of skin cancer (and it was), you have been thorough, reassuring, respectful and in every way professional.
You recognised that I had some insight into the condition of my skin and the procedures required to treat me. You listened to me. You projected expertise and compassion.
During the procedure to remove the growth you ensured that the atmosphere in the treatment room remained not only calm, but actually pleasant. Had it not been that you were excising a growth and sewing me up, I almost felt as if you, me and the nurse were at some sort of women’s discussion group. The time flew by. I had zero anxieties about the procedure and as we both know now, the wound healed flawlessly.
Thank you for your expertise and your communication skills and all round good nature. I feel very lucky.
We have replaced the images and names of real patients who provided these testimonials to protect their privacy.
The first step to feeling in charge of your skin is to book an initial consultation
FIND OUT HOW TO GET THE SKIN YOU WANT
How it works
FEEL IN CHARGE OF YOUR SKIN IN 3 EASY STEPS
STEP 1 – CALL US
STEP 2 – LET’S MEET
STEP 3 – RESOLUTION

CONTACT MY STAFF
Give us a call on 01183151178 and we’ll help guide you towards a first appointment.

MEET WITH ME
I’ll see you and examine your skin before I recommend treatment. In some cases, I can begin treating your condition on the same day.

FEEL IN CHARGE OF YOUR SKIN
I’ll guide you down the road towards a resolution of your skin condition so that you can get back to normal life.
More information about genital dermatoses
FOR THOSE WHO WANT THE DETAILS
Affiliations and memberships
I AM PROUD TO BE ASSOCIATED WITH THE FOLLOWING ORGANISATIONS
Questions and answers
RELEVANT AND INFORMATIVE VIDEOS AND ARTICLES
5 simple steps to get the clear and healthy skin you desire
With these 5 simple steps you can get the clear and healthy skin you desire. Dr Pratsou helps you to take control of your skin. Learn more...
What effect does acne have on people’s lives?
Penelope Pratsou discusses the effect of acne on people's daily lives. She explains how they feel before and after treatment. Learn more ...
What should you do if you have psoriasis?
You could be free of your psoriasis symptoms. Learn what to do if you have the skin condition and how to regain control over your skin ...

About the author
Dr Penelope Pratsou | Consultant Dermatologist
MBChB, MRCP (UK) (Dermatology)
I’m Dr Penelope Pratsou, a skilled independent Consultant Dermatologist based in Berkshire. I have specialist expertise in the diagnosis and management of all skin cancers, and in performing mole checks. I’m a trained skin surgeon and remove skin cancers, moles, skin tags, cysts and warts.
I also have invaluable experience in dealing with all skin conditions, from the common skin complaints of acne, rosacea, eczema and psoriasis, to the rarer and more complex skin problems, having seen it all through years of NHS work.
After I obtained my Membership to the Royal College of Physicians, I undertook rigorous specialist training in dermatology, before being appointed as a Consultant Dermatologist at the Royal Berkshire Hospital, Reading. There, I helped set up and lead a busy clinic for the diagnosis and treatment of suspected skin cancer. I was also actively involved in supervising and training both dermatology and GP trainees.
Alongside my increasingly busy private practice, I have maintained an NHS practice in Oxford in order to continue to engage with challenging cases and to develop my specialist interest in skin allergy.